All published articles of this journal are available on ScienceDirect.
Infective Keratitis Following Iontophoresis-assisted Corneal Crosslinking (I-CXL): A Case Report
Abstract
Introduction:
The standard corneal crosslinking (S- CXL) technique requires corneal epithelial removal, thus increasing the risk of postoperative complications. Newer technique like iontophoresis-assisted corneal crosslinking (I-CXL) with comparable efficacy as S-CXL but without the increased risk of complications associated with corneal epithelium removal is used. However, being a comparatively newer technique, the safety and efficacy of I-CXL have not been fully explored.
Case Description:
Here, we present a case of a 28-year-old woman who presented with infective keratitis in one eye after uneventful bilateral I-CXL for keratoconus. Two days after the procedure, the patient presented with decreased vision and pain in the right eye. Clinical examination revealed ciliary injection and central corneal rounded infiltrates measuring 3.0 mm × 3.0 mm with an overlying epithelial defect. Microbiological studies revealed negative results. Based on clinical examination, the patient was managed successfully with fortified topical antibiotics.
Conclusion:
To the best of our knowledge, we report the first documented case of unilateral infective keratitis following bilateral I-CXL. Ophthalmologists should monitor the possible complications post-I-CXL as it might not be as safe as we expect.
1. INTRODUCTION
Keratoconus is a progressive bilateral disease of the cornea characterized by asymmetrical and non-inflammatory thinning of the cornea. The worldwide prevalence of keratoconus is 1 in 2000; people in late childhood and early adulthood are mainly affected. Although the exact etiology is unknown, the disease is thought to be multifactorial, with genetic, environmental, and hormonal factors playing important roles [1].
Although it is a progressive disorder, in most cases, it stabilizes in the fourth decade of life. Usually, during the early years of the disease, patients are asymptomatic; however, with the progression of the disease, there is a decrease in visual acuity with the eventual significant visual loss [2]. These changes mainly occur due to myopia, astigmatism and scarring of the cornea. Although keratoconus initially shows a unilateral presentation, it eventually affects both eyes.
Corneal crosslinking (CXL) is the only minimally invasive technique available that can delay or stop the progression of the disease. This technique was developed at the University of Dresden using UVA (370 nm) and riboflavin.
CXL can be performed in different ways; one is the standard CXL (S-CXL) with debridement of the corneal epithelium (“Epi off”) and the comparatively newer technique iontophoresis-assisted CXL (I-CXL) without debridement of the corneal epithelium (“Epi on”).
In the case of S- CXL, the risk of corneal infection is high due to the debridement of the corneal epithelium. Several studies have already highlighted the similar efficacy of I-CXL compared to S-CXL with its added advantages such as the faster recovery of visual acuity and less myopia in spherical equivalent refraction after 6 and 12 months [3, 4].
However, intrastromal riboflavin concentration and transmissivity of UVA are lower in I-CXL compared to those of S-CXL [3].
Here, we present a case of infective keratitis as a complication following I-CXL in a 28-year-old female patient diagnosed with bilateral keratoconus. To our knowledge, this is the first reported case of infective keratitis following I-CXL.
2. CASE REPORT
A 28-year-old female patient presented to the ophthalmology outpatient department of King Abdullah University Hospital, Irbid, Jordan, complaining of progressive diminishing of vision in the left eye over the last 2 years.
On examination, the uncorrected visual acuity was 1.0 in the right eye and 0.5 in the left eye; the Best Corrected Visual Acuity (BCVA) in the left eye was 0.7, the manifest refraction in left eye was 0.00/ -4.00 X130.
Slit-lamp examination showed normal anterior segments except for prominent corneal nerves in both eyes; ophthalmoscopy revealed normal fundus in both eyes. Corneal thickness at the thinnest location was 434 μm and 428 μm in the right eye and left eye, respectively. Mean K was 47.5 D and 49.9 D in the right eye and left eye, respectively. Corneal tomography using Pentacam (Oculus, Wetzlar, Germany) showed a pattern consistent with keratoconus in both eyes. Krumeich stage 2 keratoconus was diagnosed in both eyes.
Progression was documented by reviewing her previous pentacam, which was done one year ago and showed 2 diopters increase in K max for both eyes. Therefore, I-CXL was planned to halt the progression of the disease.
The patient underwent I-CXL in both eyes. The procedure was carried out under sterile conditions using topical anesthesia of 0.2% oxybuprocaine hydrochloride, 1 drop administered in both eyes and repeated after 10 minutes. Starting with the right eye, the negative electrode using an annular suction ring was placed on the patient’s cornea, and the positive electrode in the form of an adhesive patch was positioned on the forehead (I-ON XL, Sooft, Montegiorgio, FM, Italy). Subsequently, the negative corneal electrode was filled with Riboflavin 0.1% (Ricrolin+, Sooft, Montegiorgio, FM, Italy)
The device was connected to a generator set at 1 mA for 5 minutes. Before UV irradiation, the device was removed, and then the cornea was irradiated with UVA at 3 mW/cm2 power for 30 min at a distance of 45 mm (VEGA CBM x-linker; C.S.O, Florence, Italy); riboflavin was reapplied at 5 minutes intervals. After the procedure, the eye surface was washed with 20 mL balanced salt solution, followed by administration of 1 drop of ciprofloxacin and a soft contact lens was placed. The same procedure was performed on the left eye.
The patient was discharged on fluorometholone 0.10% (FML) four times a day, ciprofloxacin eye drop four times a day, and lubricant eye drop four times a day for both eyes.
Two days after the procedure, the patient presented back with diminished vision (counting fingers at 30 cm), eye pain, swollen eyelids and yellowish discharge from the right eye. The patient did not report any history of trauma.
Slit-lamp examination of the right eye revealed ciliary injection; central corneal round infiltrates measuring 3.0 mm X3.0 mm with an overlying epithelial defect. Minimal epithelial edema noted around infiltrates, and +3 cellular activity in the anterior chamber with mild fibrinous reaction (Fig. 1). The contact lens that was applied after the procedure was not present.
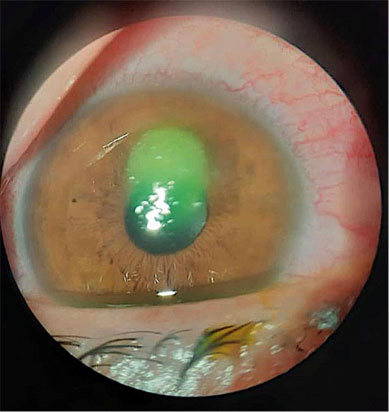
Examination of the left eye was unremarkable. Corneal scrapings were taken from the area of infiltrate in the right eye. Besides the direct microscopic examination of the scrapings following staining with Gram stain and potassium hydroxide with calcofluor white (KOH+CFW), culture was done using blood agar, chocolate agar, thioglycollate broth (THIO), and Sabouraud Dextrose Agar (SDA).
On the basis of clinical findings, the patient was managed as a case of presumed infectious keratitis. The patient was started on topical fortified vancomycin eye drops (5%; 50mg/ml) every hour alternating with topical fortified ceftriaxone (5%; 50mg/ml) in the right eye and cyclopentolate twice daily. Microbiological studies after 48 hours of incubation revealed negative culture results.
Fast clinical improvement and response to fortified antibiotics supported the diagnosis of infectious keratitis, symptoms and signs started to resolve (Fig. 2) as examined using slit lamp on the 4th-day post-presentation. The patient completely recovered by the 7th-day post antibiotic treatment with only corneal haze present at the site of infiltrates (Fig. 3).
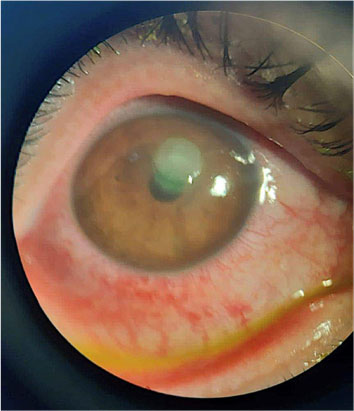
Six months post-I-CXL procedure, the patient regained pre-CXL visual acuity (1.0) in her affected eye with only mild corneal haze present.
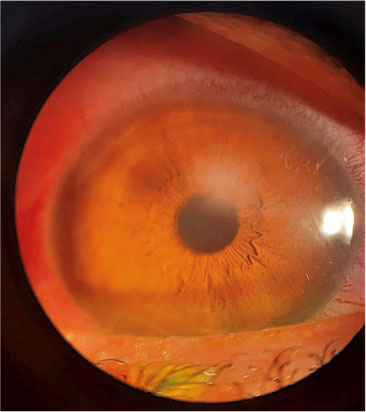
The manufacturer of the riboflavin solution (Ricrolin+, Sooft, Montegiorgio, FM, Italy) was informed, and confirmed that no similar cases of infectious keratitis following the use of their product for I-CXL were reported previously to the manufacturer.
3. DISCUSSION
Here, we have described a case of culture-negative infective keratitis in one eye in the early postoperative period 2 days following I-CXL in both eyes; the patient was managed successfully with fortified antibiotics. Although there are cases of infective keratitis following CXL, none of them were associated with I-CXL [5, 6].
Several studies have already documented the long term improvement of keratoconus following CXL [4]. However, there are various complications of CXL reported like postoperative eye pain, infective keratitis, abnormal wound healing, corneal haze, corneal edema, peripheral sterile infiltrates, reactivation of herpes simplex virus, and finally, failure of treatment [5].
Debridement of corneal epithelium is one of the most important causes of most of the common complications following CXL (“the epi off”). Bacterial keratitis due to E. coli, Streptococcus salivarius, Streptococcus oralis, and coagulase-negative Staphylococcus species, Staphylococcus epidermidis, and Pseudomonas aeruginosa were reported in different studies [6].
Therefore, to avoid the above-mentioned complications associated with the “epi off” CXL and at the same time, facilitating the diffusion of riboflavin through the intact corneal epithelium, different “epi on” strategies have been developed [7]. In I-CXL, the non-invasive entry of riboflavin is facilitated through the intact corneal epithelium with the help of electric current (iontophoresis) [7]. The major advantages of I-CXL over CXL are avoidance of complications related to epithelium debridement (especially postoperative infective keratitis), besides faster recovery of vision and less myopia [7].
Microbial keratitis is a serious ocular condition and is considered as sight-threatening condition, especially in developing countries [8]. Isolation of the causative agent by culture technique remains the gold standard for microbial keratitis [8]. Isolation of microorganisms is essential for choosing the appropriate drug, avoiding the emergence of antibiotic resistance due to empirical therapy, and getting favorable clinical outcomes within a short span of time.
However, despite best efforts, culture-negative keratitis contributes to approximately 30-40% of cases of infectious keratitis [9]. Prior antibiotic therapy is the most common cause of culture-negative keratitis; hence at the time of corneal scraping, there is a high chance that the disease is already in the phase of recovery following antibiotic therapy; however, patients usually respond well to empirical antibiotic therapy and rarely require surgical interventions [9].
In the reported case above, following the I-CXL procedure, the patient was prescribed prophylactic ciprofloxacin eye drops to avoid bacterial infection. After 2 days, she presented with symptoms and signs in the right eye suggestive of infectious keratitis; however, the culture of corneal scrapings from the affected eye was negative. The most likely cause of negative culture reports is possibly the prior antibiotic therapy. The patient's symptoms resolved following topical fortified vancomycin and ceftriaxone therapy.
Although the patient did not report any history of trauma, minor trauma could have been inflicted during suction ring application or by the tip of the eye dropper during the administration of her postoperative medications. Moreover, epithelial disruption was demonstrated in some patients in a study that evaluated epithelial integrity post transepithelial CXL [10] therefore it might be advisable to pay attention to epithelial integrity post I-CXL.
CONCLUSION
To conclude, despite the advantages of intact corneal epithelium, compared to S- CXL, I-CXL might not be completely safe as there might be a risk of postoperative complications like infective keratitis. Until both the safety and efficacy of I-CXL are well established through further studies, ophthalmologists should monitor for potential postoperative complications, if any, following I-CXL.
LIST OF ABBREVIATIONS
| S-CXL | = Standard Cross-Linking |
| I-CXL | = Iontophoresis Cross-Linking |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Written consent was obtained from the patient.
STANDARDS OF REPORTING
This article was written in accordance with CARE guidelines and methodologies.
AVAILABILITY OF DATA AND MATERIALS
The data sets used during the current study can be provided from the corresponding author (N.A) ,upon reasonable request.
FUNDING
None.
CONFLICT OF INTERESTS
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


