All published articles of this journal are available on ScienceDirect.
A Case of Papillophlebitis Caused by the Contraceptive Implant in a Healthy Young Woman with Angioid Streaks
Abstract
Introduction:
Papillophlebitis is a rare condition that has a high probability of misdiagnosis due to its puzzling resemblance to common conditions, especially Central Retinal Vein Occlusion (CRVO) and papillitis.
Methods:
We present an interesting case of a 30-year-old healthy woman with mild CRVO in the right eye associated with ocular pain on upgaze, visual field defect, dyschromatopsia, and desaturation of red color along with initially normal visual acuity, nondetectable relative afferent pupillary defect, and normal foveal reflex. She underwent a subdermal etonogestrel implant (progestin) by a gynecologist two months before presentation. Following the removal of the progestin implant by her gynecologist, we started the patient on intravenous methylprednisolone (500mg daily for 3 days).
Results:
This combination of incomplete features of CRVO and papillitis guide us to the diagnosis of atypical papillophlebitis. The fundi showed a typical appearance of angioid streaks. The association between papillophlebitis and angioid streaks was unclear. After a thorough review of the literature, no correlation was found, indicating that angioid streak is only an incidental finding.
Conclusion:
The patient’s condition improved with systemic steroid administration, and complete visual recovery was noted after one year, despite the presence of macular ischemia and nerve fiber layer atrophic changes on Optical Coherence Tomography (OCT) and OCT angiography.
1. INTRODUCTION
Papillophlebitis is an optic nerve head swelling with a presentation similar to mild Central Retinal Vein Occlusion (CRVO). It affects individuals aged less than 50 years, leading to a mild decrease in visual acuity. The major findings besides disk swelling include perivenous retinal hemorrhages and dilatation and tortuosity of retinal veins. Although corticosteroids are used in the treatment, the condition may improve spontaneously after several months [1].
Papillophlebitis is a rare condition characterized by a high probability of misdiagnosis because of its similarity to other common conditions. Lyle and Wybar reported it for the first time in 1961; since then, various descriptions had been given to this distinctive entity, such as retinal vasculitis [1], papillophlebitis [2, 3], benign retinal vasculitis [4], optic disk vasculitis [5], venous papillopathy [6], and big blind spot syndrome [7]. In 1972, Hayreh [5] had classified papillophlebitis into two types: type I, which is characterized by disk edema similar to papillitis with minimal retinal pathology that responds well to systemic steroids, and type II, where CRVO is present, with a slight response to systemic steroids.
2. CASE PRESENTATION
A 30-year-old healthy woman presented with paracentral blurring in the right eye associated with a migraine-like headache for 5 days. Past medical history was unremarkable apart from an etonogestrel implant (progestin) two months before presentation. Ophthalmic examination revealed Best-Corrected Visual Acuity (BCVA) of 20/20 in both eyes, mild pain on upgaze, paracentral scotoma by confrontational visual field test, and mild red desaturation in the right eye. No Relative Afferent Pupillary Defect (RAPD) was detected besides normal ocular motility on anterior segment examination.
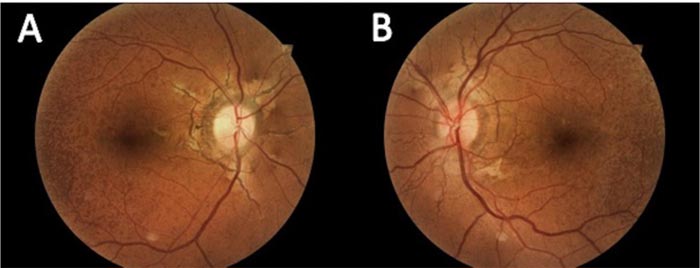
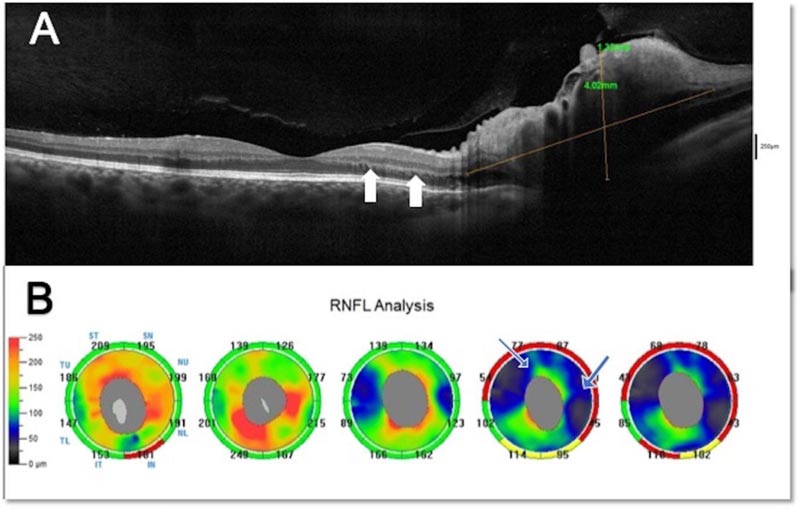
Fundus examination showed swelling of the optic nerve head with blurry margins, venous tortuosity, and flame-shaped hemorrhages in four quadrants of the right eye. Additionally, angioid streaks were noted bilaterally (Fig. 1A-D). Apart from the angioid streaks, the left eye fundus was normal (Figs. 2A and B). Optical Coherence Tomography (OCT) angiography revealed right optic disk swelling besides normal left optic disk, normal maculae, and absence of choroidal neovascularization (Fig. 3A). OCT cornea showed thin corneas with a central corneal thickness of 483 μm in both eyes. Blood tests, including complete blood count, erythrocyte sedimentation rate, lipid profile, fasting blood sugar level, and HbA1c level, were all within normal limits. The patient has cut off her visits and then returned after 1 month.
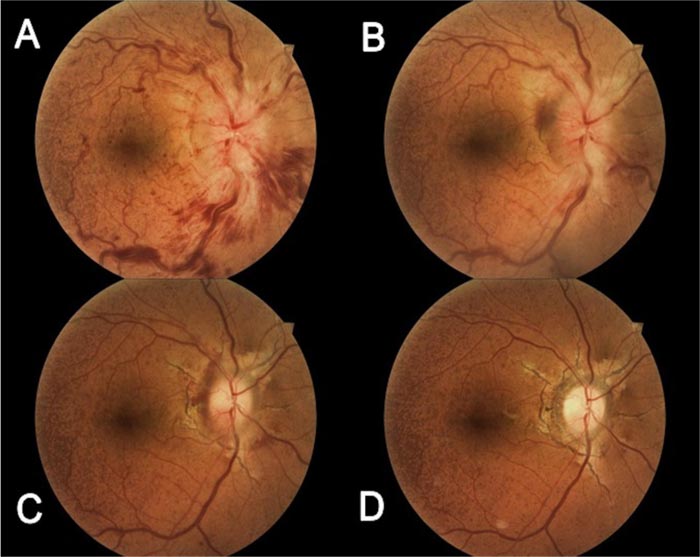
On presentation, a reduction of the BCVA to 20/100 was noted with mild pain on dextroelevation in the right eye, and no RAPD was detected. Fundus examination showed a mild resolution of venous congestion and faint collateral vessels near the (OD) (Fig. 1B). Additionally, OCT angiography results were within normal limits. We decided to refer the patient to her gynecologist to remove the etonogestrel implant then we treated her with three doses of 500 mg intravenous methylprednisolone for 3 days.
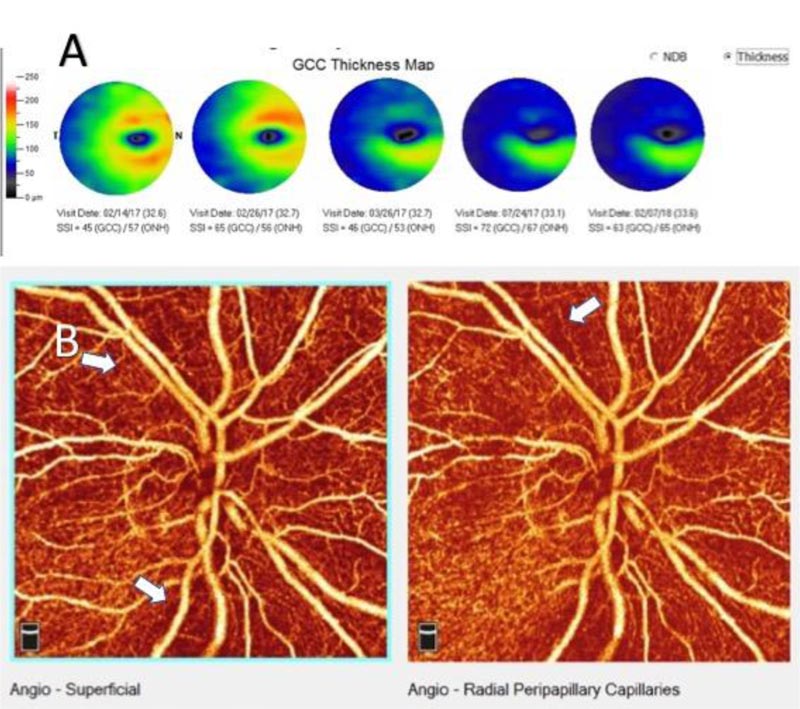
The patient was lost to follow-up again for 4 months. On presentation, BCVA improved to 20/32 besides total resolution of all retinal hemorrhages and optic disk swelling in the right eye. Nevertheless, mild optic disk pallor with tiny collaterals was noted. OCT revealed atrophic macular changes nasally with pathological loss of peripapillary nerve fiber layer (Fig. 3B); in addition, OCT angiography showed peripapillary areas of diffuse capillary nonperfusion. After one year, the BCVA had retained to normal, and the rest of the examination was unremarkable, apart from the mild pallor of the optic nerve head (Fig. 1D) and ganglion cell complex (Figs. 4A and B).
3. RESULTS AND DISCUSSION
Papillophlebitis is a rare condition that affects the young population and usually has an excellent prognosis [4], with or without treatment [5, 8]. The pathophysiology of papillophlebitis is unclear, and many theories were suggested. In 1961, Lyle et al. suggested an inflammatory mechanism that caused occlusion within the central retinal vein and considered it a form of Eales disease [1]. In 1966, Lonn and Hoyt attributed it to inflammation in the vein adjacent to the optic nerve head [2].
Our case represents an unusual finding of angioid streaks with papillophlebitis that was associated with pain on eye movements and headache for 3 months. The visual acuity was normal on presentation. However, a sudden decrease in the visual acuity was noted after 2 weeks. In this particular case, removal of the etonogestrel implant (progestin) was advised as it could be a risk factor for vascular thrombosis, CRVO, and papillophlebitis [9, 10]. Due to the rapid deterioration of visual acuity in the right eye, we commenced intravenous methylprednisolone to treat possible inflammation associated with papillophlebitis [6]. Although the patient had not attended regular follow-ups for approximately 3 months, visual acuity improved to 20/32 following intravenous steroid administration and contraceptive implant removal. In the next 8 months of regular visits, vision in the right eye continued to improve and finally returned to 20/20.
The rare presentation of angioid streaks and CRVO was previously reported. In 1979, Deutman presented a case of peripapillary Choroidal Neovascular Membrane (CNVM) and CRVO in angioid streaks, attributing it to the pressure induced by the peripapillary CNVM on the adjacent retinal vein [11]. In our case, no peripapillary pathology was detected, and the use of a contraceptive implant was the only acceptable explanation for the development of papillophlebitis. Therefore, most probably, the angioid streak is an incidental finding.
We have reviewed the literature for cases of papillophlebitis in patients with angioid streaks, but no similar cases were found. Thus, we believe that this is the first case that presents this incidental finding.
CONCLUSION
Implantable progestin is the cause of papillophlebitis in this young, healthy woman, and no association was found between angioid streaks and papillophlebitis in this case. Papillophlebitis has a favorable prognosis even with the development of unusual nerve fiber layer thinning, areas of capillary nonperfusion, and optic nerve head pallor.
The improvement of the condition with systemic steroid administration is in accordance with the theory of inflammatory mechanism that occurs in this entity.
AUTHORS' CONTRIBUTIONS
MA: Mohammad Abusamak, HR: Hamzeh Alrawashdeh
Substantial contribution to conception and design
MA, HR Substantial contribution to acquisition of data
MA Substantial contribution to analysis and interpretation of data
MA, HR Drafting the article
MA, HR Critically revising the article for intellectual content
MA Final approval of the version to be published MA
LIST OF ABBREVIATIONS
| BCVA | = Best-Corrected Visual Acuity |
| CNVM | = Choroidal Neovascular Membrane |
| CRVO | = Central Retinal Vein Occlusion |
| RAPD | = Relative Afferent Pupillary Defect |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Written informed consent was obtained from the patient.
AVAILABILITY OF DATA AND MATERIALS
The data sets used during the current study can be provided from the corresponding author (M.A), upon reasonable request.
STANDARDS OF REPORTING
CARE guidelines have been followed.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
FUNDING
None.
ACKNOWLEDGEMENTS
The authors acknowledge Dr. Emad Alshekh Khaled for performing the clinical examination for this case.


