All published articles of this journal are available on ScienceDirect.
Subconjunctival Air Leakage After Descemet's Stripping Automated Endothelial Keratoplasty(DSAEK) in a Post-Trabeculectomy Eye
Abstract
Purpose: To report a case of subconjunctival air leakage from the anterior chamber (AC) into a trabeculectomy bleb after Descemet's stripping automated endothelial keratoplasty (DSAEK).
Methods: An 89 year-old woman with a previous history of primary open angle glaucoma in her left eye and previous trabeculectomy with mitomycin C had DSAEK on the patient’s left eye in order to treat her endothelial disease. During the DSAEK procedure, air was injected into the AC to aid in graft adherence.
Results: The day after the surgery, subconjunctival air leakage from the AC into a trabeculectomy bleb was observed.
Conclusion: Although our patient did not have any complications from this leak, there exists the potential for hypotony, bleb-related infections, and dislocations of the DSAEK graft. Given the potential consequences, these patients should be monitored closely.
INTRODUCTION
Descemet's stripping automated endothelial keratoplasty (DSAEK) is currently the most popular method for selective endothelial keratoplasty [1-3]. Fewer complications are expected when posterior corneal tissue is selectively replaced because full thickness penetrating keratoplasty (PKP) can be complicated by a variety of postoperative problems and can lead to corneal structural instability. Currently, most surgeons utilize an air bubble to tamponade donor corneal tissue to the host cornea at the conclusion of DSAEK procedures. In this case report, we aim to report a case of subconjunctival air leakage from the anterior chamber (AC) into a trabeculectomy bleb after DSAEK.
CASE DESCRIPTION
An 89 year-old woman with a previous history of primary open angle glaucoma in her left eye and previous trabeculectomy with mitomycin C (MMC) presented to our clinic with bullous keratopathy and band keratopathy. Her intraocular pressure (IOP) was well controlled (10 mmHg) with a topical beta-blocker. The remainder of her ophthalmic and general exam was otherwise normal. We performed DSAEK on the patient’s left eye in order to treat her endothelial disease.
At the end of her routine and uneventful DSAEK surgery, sterile filtered air was injected into the AC to tamponade the donor graft into position. On post-operative day one, slit lamp examination revealed subconjunctival air leakage inside the trabeculectomy bleb (Fig. 1). The DSAEK graft was well centered and adherent to the host stoma with a 50-60% air fill remaining. IOP measured 14 mmHg and the remainder of her ocular exam was within normal limits.
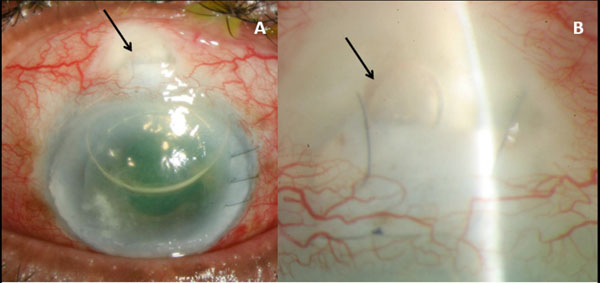
Fig. (1). Low (A) and high power (B) slit lamp photographs of the left eye on post-operative day one demonstrates subconjunctival emphysema (arrows) in the trabeculectomy bleb after Descemet's stripping automated endothelial keratoplasty (DSAEK).
DISCUSSION
DSAEK is an effective means for endothelial keratoplasty that preserves structural integrity of the cornea. Currently, an AC air bubble is used to tamponade the graft into the proper position in most cases. In a patient who has a functional filtering bleb, it is possible for the AC air to travel through the filter and into the conjunctival bleb.
There are several potential complications stemming from air movement from the AC into the trabeculectomy bleb. First, the DSAEK procedure could fail. Air is injected into the AC to tamponade and position the DSAEK graft into the proper anatomic location. If enough air is not left in the AC, there is a potential for graft dislocation and DSAEK failure, though some doctors now remove the air from the AC just before completion of the procedures [4]. Additionally, air travelling though a trabeculectomy filter may lyse functional adhesions that have formed and alter the rate of aqueous filtration through the bleb. This could result in overfiltration, a flat AC, and hypotony. If the AC becomes very shallow, there is a possibility of iris-cornea touch that could damage the newly transplanted endothelium affect the success of the DSAEK surgery.
Subconjuctival air bubble could also lead to an increased risk of bleb-related infections due to an enlarged tract and an increased flow rate between the AC and the conjunctival bleb. Lastly, a large amount of air could cause avascular mitomycin C treated blebs it to fail due to barotraumas or overfiltration.
Even without any pressure from subconjunctival air, early- and late-onset bleb leak and its associated hypotony are among the most common complications after trabeculectomy [5, 6].
Although our patient did not suffer any of these potential complications and the air spontaneously resolved, one should follow similar patients closely to monitor for these changes. Some authors have suggested that air may be toxic to endothelium [7, 8]. Therefore, the optimal solution may be to forgo the use of any AC air in patients who have a functional filtering bleb; however, the risk of post-operative DSAEK graft dislocation may increase.


