All published articles of this journal are available on ScienceDirect.
Corneal Microstructural Analysis in Weill-Marchesani Syndrome by In Vivo Confocal Microscopy
Abstract
A thick cornea is a constant ocular finding in the mesodermal dysmorphodystrophy (Weill-Marchesani Syndrome). In this study we investigated with confocal microscopy, the corneal structure in vivo in the patient affected by Weill-Marchesani Syndrome (WMS) in an attempt to explain the thickness increment. The corneal study showed in both eyes a highly increased central thickness with normal topography and sensitivity. The confocal examination revealed an increased evidence of keratocytes in the anterior stroma with abnormal and activated appearance. The mid and deep stroma and endothelial layer were normal. These confocal findings are a newly described feature of corneal involvement in WMS. The increase of the corneal thickness in the affected patient maybe associated with connective tissue alterations, such as abnormal collagen synthesis, that characterizes the disease.
INTRODUCTION
Weill-Marchesani Syndrome (WMS), also called mesodermal dysmorphodystrophy, is a systemic connective tissue disorder related to the altered encoding for protein of extracellular matrix with fibrous tissue hyperplasia [1]. The disease is genetically determined with both autosomal dominant and recessive inheritance modalities and exhibit clinical homogenous features, despite genetic heterogeneity. The diagnosis is based on clinical findings such as short stature, brachycephaly, stiff joints; ocular abnormalities include short axial length, shallow anterior chamber, microspherophakia, with high lenticular myopia, and ectopia lentis [2]. The constant corneal finding is an increased central thickness, of yet unexplained origin [2, 3].
In this study we have investigated the corneal structure by in vivo confocal microscopy, in a patient with WMS, in the attempt to explain the thickness increment. As to our knowledge this is the first report concerning corneal in vivo confocal examination in eyes with WMS.
CASE REPORT
We examined a 19-year-old male referred to the Cornea Unit of the Ophthalmology Clinic of the University of Messina, Messina, Italy, to undergo laser refractive surgery. The patient presented with short stature, high myopia, thick cornea (618 microns in the RE and 622 microns in the LE), shallow anterior chamber (2.75 mms and 2.55 mms respectively), small thick lens (5.0 mms and 4.9mms in the RE and LE), and short axial length (22.01 mms and 21.97 mms). On the basis of these findings the clinical diagnosis of WMS was posed. The patient was a soft contact lens wearer up to two month prior to the visit.
The corneal structure was examined by confocal microscopy (Confoscan 4, Nidek Technologies, Italy). Confocal investigation showed normal epithelial layers characterized by basal cells with bright borders and dark cell bodies and well represented superficial nerves (Fig.1A, B). In the anterior stroma, the keratocytes shape varied showing small and elongated cells with irregular bodies, frequently clustered and activated (Fig. 1C, D); the mid and deep stroma were normal (Fig. 1E). We considered ten photographs of anterior and posterior stroma of each eye to determine the keratocytes density. It was found to be 1228.2 ± 77.15 cell/mm2 in the anterior stroma of the RE and 1180.35 ± 63.54 cell/mm2 in the LE; in the posterior stroma it was 582.07± 75.47 cell/mm2 in the RE and 583.75 ± 29.89 cell/mm2 in the LE. Corneal endothelium was normal in both eyes with the mean cell density of 3461 cell/mm2 in the RE and 3405 cell/mm2 in the LE respectively (Fig. 1F).
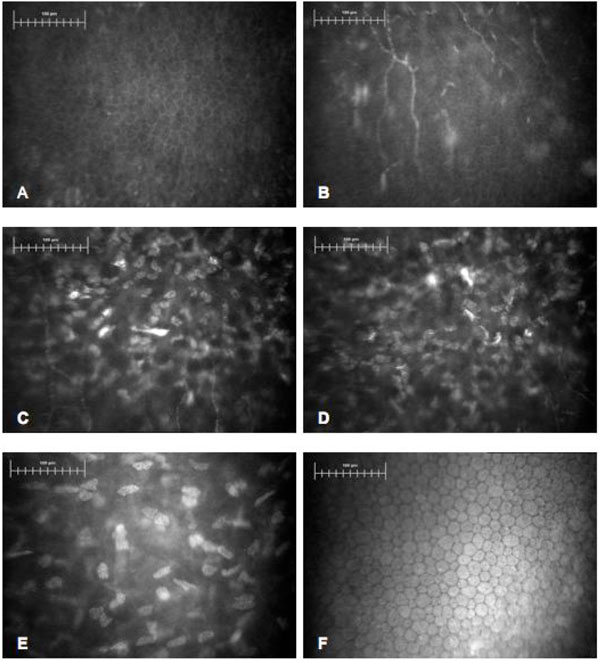
Confocal images in WMS patient. Bar represents 100μm. (A) Normal basal epithelium with dark cell bodies and bright borders. (B) Sub-epithelial layer with normal nerves fibers. (C, D) Superficial stroma. Abnormally shaped, clustered keratocytes with presence of activated cells. (E) Deep stroma with normal keratocytes. (F) Corneal endothelium with normal cell morphology and density.
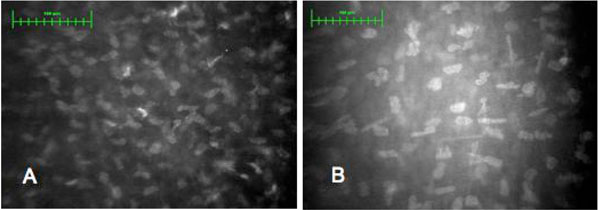
Confocal images in normal eye. Bar represents 100μm. (A) Superficial stroma. (B) Deep stroma.
Furthermore, we have examined 10 eyes of 10 age matched healthy subjects who were soft contact lenses wearers, to compare the confocal corneal findings. In this group the mean keratocyte density in the anterior stroma resulted to be 760.4 cell/mm2 and in the posterior stroma 563.6 cell/mm2 respectively (Fig. 2A, B).
DISCUSSION
Ocular findings such as short axial length, shallow anterior chamber, and thick lens were already described in WMS as well as the excessive corneal thickness, the origin of which is unknown. The purpose of this study was to investigate the cornea in vivo, by confocal microscopy, in the attempt to identify the changes that might help to explain corneal features in WMS [2, 3]. Confocal microscopy showed normal endothelium and deep stroma. The normality of the corneal endothelium, responsible for corneal hydratation and transparency maintenance is relevant because it allows the exclusion of endothelial involvement in the CCT increase in WMS. The main confocal finding is the abnormal cell population in the superficial stroma, consisting of activated and abnormally shaped keratocytes with an increased density. In fact the reported normal values for normal population are between 804±15 cell/mm2 to 1060±47 cell/mm2 for the anterior stroma and 480±67 cell/mm2 and 771±14 cell/mm2 for the posterior stroma, respectively [4]. The keratocytes density calculated in both anterior and posterior stroma in the control group exhibited such normal values. Therefore, it appears that in our patient, beside a normal cellular population in the posterior stroma, there is an alteration of the cellular pattern localized in the anterior stroma.
Beside the increased keratocytes density the presence of activated cells acquiring fibroblastic characteristics could indicate an increased metabolic activity and collagen synthesis. As an abnormal collagen synthesis is at a basis of WMS, the abnormalities of the anterior corneal stroma evidenced in this study, could possibly be attributed to the connective tissue alterations that characterize the disease, and help to explain the increase of the corneal thickness in affected patients. This is the first report of in vivo confocal corneal investigation in mesodermal dysmorphodystrophy. Further investigations involving a larger number of WMS subjects would be useful to confirm the anterior stroma alterations in the cornea of the affected patients.


