All published articles of this journal are available on ScienceDirect.
Characteristics of Sympathetic Ophthalmia in a Single International Center
Abstract
Aim:
To report the main features of sympathetic ophthalmia in a referral ophthalmology center.
Methods:
Retrospective clinical study. We reviewed clinical records of patients with diagnosis of sympathetic ophthalmia attending the Uveitis Department from 2007 to 2013. Patients were selected by clinical criteria. Descriptive statistics were used to assess variables.
Results:
Twenty patients were included for analysis, 13 males and 7 females. Mean follow up was 1 year. The median age of presentation was 50 years. Fifty percent had history of ocular trauma and 50% had history of intraocular surgery, of which 40% underwent phacoemulsification. The time between injury and onset of symptoms ranged from 1 to 456 months. Most common ocular manifestations were mutton fat keratic precipitates and anterior chamber inflammation. All patients received oral prednisone as single or combined therapy. Sixty percent of the sympathizing eyes improved two or more lines of vision and 20% lost two or more lines of vision.
Conclusion:
This report from a single center adds to the body of literature of sympathetic ophthalmia occurring in a specific population. Our data found a high proportion of patients with sympathetic ophthalmia after phacoemulsification.
INTRODUCTION
Despite the first complete clinical description by William Mackenzie of sympathetic ophthalmia performed in 1840, its cause has not been completely understood, although an autoimmune reaction of exposed ocular antigens is implicated, causing a bilateral granulomatous uveitis involving an eye exposed to trauma or surgery (inciting eye) and the fellow eye (sympathizing eye) [1, 2].
It is a rare disease, with an estimated incidence of 0.03/100,000 in a study population over 15 months [3]. Despite that fact, the importance in knowledge of sympathetic ophthalmia is that, this entity is a sight-threatening illness with one third of the patients ending with a final visual acuity of 20/200 or worst, and requiring fast and aggressive anti-inflammatory therapy to try to improve the visual outcome [4].
Some case series have been reported, with slight variations between populations. The goal of this study is to report the characteristics of patients with sympathetic ophthalmia in a referral center in Mexico in a period of seven years.
MATERIALS AND METHODS
This is an observational and retrospective clinical study; we reviewed the clinical data of all patients with a diagnosis of sympathetic ophthalmia attending the Department of Uveitis and Ocular Immunology at Instituto de Oftalmologia “Conde de Valenciana” in Mexico city from 2007 to 2013.
The diagnosis of sympathetic ophthalmia was performed clinically; patients presented with the history of previous ocular trauma or surgery and a bilateral granulomatous uveitis, associated with anterior inflammation with mutton-fat keratic precipitates and posterior findings like vitritis, choroiditis, optic nerve swelling and serous retinal detachment in some cases (Figs. 1 and 2) [5]. A thorough lab investigation was performed in all patients to rule out other causes of ocular inflammation.
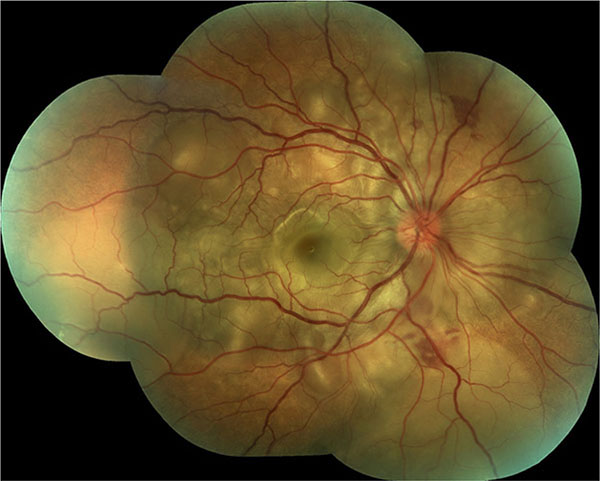
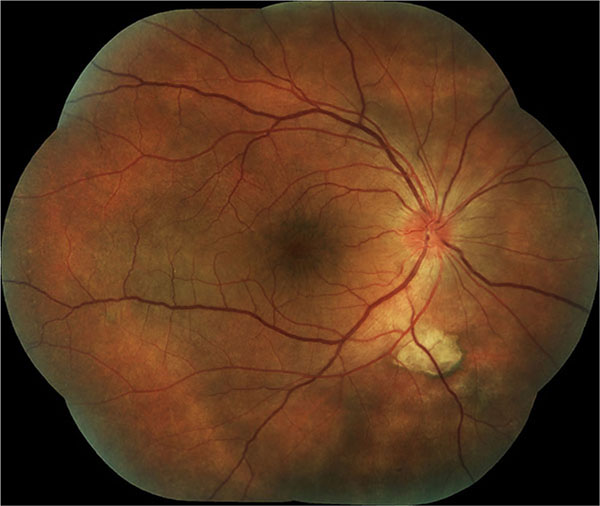
After the patients met our criteria, information was searched in the clinical records for: gender, age, symptoms, type of injury (trauma or surgery), type of surgery (if applicable), visual acuity in the inciting eye in their first and last consultation, visual acuity in the sympathizing eye in their first and last consultation, findings in examination, treatment received and progression of inciting eye to ptisis bulbi. The main outcome was final visual acuity. Approved informed consent was obtained from all patients undergoing immunosuppressive therapy.
Using descriptive statistics, categorical variables were evaluated using percentages and numerical variables were assessed using measures of central tendency for non-parametric distribution. Data were represented in tables.
RESULTS
A total of 42 patients with diagnosis of sympathetic ophthalmia were found. However, we had to exclude 22 patients, 12 because of insufficient data in their files, and 10 because they did not fulfill our clinical criteria for sympathetic ophthalmia; then 20 patients were included for analysis. The individual characteristics of the patients are shown in Table 1.
| Patient | Age (years) | Sex | Triggering Event | Sympathetic Eye | Inciting Eye | ||
|---|---|---|---|---|---|---|---|
| Initial VA (LogMAR) |
Final VA (LogMAR) |
Initial VA (LogMAR) |
Final VA (LogMAR) |
||||
| 1 | 52 | F | Surgery | 0 | 1.30 | NLP | NLP |
| 2 | 56 | F | Surgery | 1 | 0.48 | NLP | NLP |
| 3 | 58 | F | Surgery | 0.40 | 0.30 | NLP | NLP |
| 4 | 72 | M | Trauma | 3 | 0.70 | 2 | 3 |
| 5 | 18 | M | Trauma | 0.18 | 0.18 | 3 | NLP |
| 6 | 68 | F | Trauma | 0.40 | 0.18 | 3 | 3 |
| 7 | 25 | F | Surgery | 0 | 0.10 | 3 | NLP |
| 8 | 50 | F | Surgery | 3 | 0.10 | 0 | NLP |
| 9 | 55 | M | Surgery | 0.40 | 0 | 3 | 0.60 |
| 10 | 62 | M | Surgery | 3 | 2 | NLP | NLP |
| 11 | 74 | M | Surgery | 0.70 | 1.30 | 3 | NLP |
| 12 | 75 | M | Surgery | 1.30 | 2 | 1 | 0.30 |
| 13 | 38 | M | Trauma | 0 | 0 | 3 | NLP |
| 14 | 43 | M | Trauma | 1.30 | 0.60 | NLP | NLP |
| 15 | 52 | M | Trauma | 1.30 | 1 | 3 | 3 |
| 16 | 18 | M | Trauma | 1.60 | 0 | 3 | 3 |
| 17 | 19 | M | Trauma | 0.60 | 0 | NLP | NLP |
| 18 | 31 | F | Trauma | 0.10 | 0.30 | 3 | 3 |
| 19 | 72 | M | Trauma | 0.54 | 0.30 | NLP | NLP |
| 20 | 62 | M | Surgery | 3 | 0.18 | 3 | 3 |
The average age at presentation was 50 ± 19.3 years (range from 18 to 75 years), with 13 men (65%) and 7 women (35%). The number of consultations for the patients in the period of time of our study was an average of 13.75 ± 20.4 visits per patient (range 2 to 72 visits). According to the injury, there were 10 patients (50%) with previous history of trauma, and 10 patients (50%) who underwent ocular surgery. In the surgery group, 4 patients (40%) underwent phacoemulsification with intraocular lens implantation, 3 (30%) retinopexy for retinal detachment, 1 patient (10%) extracapsular cataract extraction with intraocular lens implantation, 1 (10%) underwent congenital cataract extraction surgery with aphakia, and 1 patient (10%) an Ahmed valve implantation. The inciting eye presented as phthisis bulbi in 7 patients (35%); five of them were from the group of a previous ocular surgery and two in the group of trauma. In 8 (40%) of our patients, the inciting eye was the left eye, and in 12 (60%) of them was the right eye.
All the patients (100%) consulted referring progressive decreased vision in the sympathizing eye, and two of them (10%) also had foreign body sensation in this same eye. The time between the injury and the onset of symptoms ranged from 1 month to 456 months, with an average of 104.45 months (8.7 years).
Table 2 presents the frequency of patients with a visual acuity of 20/50 or worse and 20/200 or worse in the inciting and sympathizing eye at presentation and at last consultation. The median visual acuity in the inciting eye at presentation was of hand motion (range 20/20 to no light perception), with 7 patients (35%) having a visual acuity of no light perception. The median visual acuity in the sympathizing eye at presentation was of 20/80 (range 20/20 to hand motion), with 4 patients (20%) having a visual acuity of hand motion.
| Inciting Eye Number of patients (%) |
Sympathizing Eye Number of patients (%) |
|
|---|---|---|
| Visual acuity of 20/50 or worse at presentation | 19 patients (95%) | 15 patients (75%) |
| Visual acuity of 20/200 or worse at presentation | 19 patients (95%) | 9 patients (45%) |
| Visual acuity of 20/50 or worse at last consultation | 19 patients (95%) | 8 patients (40%) |
| Visual acuity of 20/200 or worse at last consultation | 18 patients (90%) | 5 patients (25%) |
The most common ocular manifestations were mutton-fat keratic precipitates (Fig. 3) and anterior chamber reaction that were present in all patients. The ocular manifestations in the group of patients are enlisted in Table 3.

| Manifestation | Number (%) |
|---|---|
| Mutton-fat keratic precipitates | 20 (100%) |
| Anterior chamber inflammation | 20 (100%) |
| Vitritis | 12 (60%) |
| Serous retinal detachment | 5 (25%) |
| Dallen-Fuchs nodules | 5 (25%) |
| Choroiditis | 4 (20%) |
| Optic nerve swelling | 1 (5%) |
| Iris nodules | 1 (5%) |
| Retinal vasculitis | 1 (5%) |
| Serous choroidal detachment | 1 (5%) |
Regarding treatment, patients received a variety of medications. All the patients received initially prednisone in oral administration at 1mg/kg/day. From the topical medications, 20 patients (100%) were treated initially with drops of 1% prednisolone in tampering doses and 3 patients (15%) with topical non-steroidal anti-inflammatory drugs. Three patients (15%) were given regional steroids with periocular drug administration of 1 ml of betamethasone. Posteriorly during the course of the disease, some patients required other types of immunosuppressive agents, and 5 patients (25%) received methotrexate, 4 patients (20%) azathioprine and 3 patients (15%) received oral cyclophosphamide.
The median visual acuity in the inciting eye at the last consultation was of no light perception (range 20/40 to no light perception) because 12 patients (60%) had a visual acuity of no light perception. The median visual acuity in the sympathizing eye at the final consultation was of 20/40 (range 20/20 to counting fingers at 2 feet). In the sympathetic eye, we found that 12 patients (60%) improved two or more lines in visual acuity from the first to last consultation and one patient (5%) improved one line of vision. On the other hand, four patients (20%) deteriorated their visual acuity by two or more lines of vision and one patient (5%) lost one line of visual acuity, between first and last consultation. Finally, two patients (10%) didn't show any improvement or deterioration in their visual acuity. No patient had enucleation and no new cases of phthisis presented at any moment of the follow-up. The median follow-up time was 1 year (range 1 to 5 years).
DISCUSSION
In this study, we present the characteristics of patients with sympathetic ophthalmia in a reference center in Mexico. Our findings are consistent with previous studies in that the majority of the patients in the study group are men [6, 7]. It is suggested a slight predilection toward males that could be attributed to the increased exposure to trauma.
Although previous studies estimated that the prevalence of sympathetic ophthalmia after ocular trauma, from 0.1% to 0.3%, is higher than the 0.02% prevalence after ocular surgery, a prospective surveillance in a specific population established that surgery, particularly the retinal surgery, is the most important risk factor [3]. Interestingly, our group of patients showed a half and half proportion between the patients with trauma and the patients with surgery, most of them phacoemulsification with intraocular lens implantation (40%), and only 30% had retinal surgery, none had a vitrectomy. This may be due to the important disproportion of surgeries in the setting of the study, because the number of cataract surgery are much higher compared with the retina surgeries, although a prospective study could detect undiagnosed sympathetic ophthalmia in the group of vitrectomy.
None of our patients in the ocular trauma group had early enucleation after the event, which may be due to a conservative treatment principle present in the study center. Also, no patients were enucleated at the follow-up, as the benefit of enucleation after the onset of sympathetic ophthalmia remains unclear [2].
After the inciting event, traumatic or surgical, intraocular inflammation has been reported in a wide range between 1 week and 66 years, with 80% of the cases occurring within 3 months after injury to the exciting eye and 90% within 1 year [6, 8]. In our group of patients, the patient who developed the disease in the shortest time was within 1 month and the longest time 38 years after injury.
Compared with a multicenter study, we found that the visual acuity in the inciting eye at presentation was similar in our group, because 95% of our patients had a visual acuity of 20/50 or worse, compared to 94% of them, and 95% of our patients had 20/200 or worse, compared to 92% of them [9]. Not in the same way, our patients had a worst visual acuity in the sympathizing eye at presentation, with a visual acuity of 20/50 or worse in 75% of patients, compared to 46% in their group, and a visual acuity of 20/200 or worse in 45% of patients, compared to 26% [9]. This could be explained because our uveitis department represents a reference center, wich may involve patients with more advanced disease.
The anterior chamber inflammation was present in all the patients from our series, which was also the most common clinical feature of another series [3]. The Dallen-Fuchs nodules that is considered a classic but not pathognomonic sign of sympathetic ophthalmia, was present in only one fourth of the patients.
The leading course of treatment with our patients was the systemic and topical steroids, as we treated all our patients with oral prednisone and drops of prednisolone. We treated three of our patients with regional steroids in a periocular injection form, which according to some authors; this localized treatment may have a potential benefit, as it allows for high concentrations of medication to be delivered directly to the eye, avoiding the harmful side-effects of systemic medication [10]. We also used immunosuppressive therapy in an important proportion of patients, as we consider that these agents help in refractory cases and to avoid the adverse effects of high-dose steroids [5, 11]. The immunosuppressive therapy have demonstrated good results in other uveitic pathologies [12]. Other treatments like a high-dose chlorambucil therapy [13] and a fluocinolone acetonide implant [14] have been tested with successful results by other authors.
Compared with the previously mentioned multicenter study, despite the difference in the visual acuity at presentation, the visual acuity at the end of the follow-up in the sympathizing eye was 20/50 or worse in 40% of our group of patients, that is similar to the 41% of their group, and 20/200 or worse in 25% of the patients in both groups [9]. We got relative good results as 65% of our patients improved one or more lines of vision.
Some limitations of this study are, the small number of patients and that all of them are from a single center, and also that the diagnosis of sympathetic ophthalmia was done only with clinical criteria and no with a histologic diagnosis. This study adds to the body of literature of sympathetic ophthalmia occurring in a specific population.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.


