All published articles of this journal are available on ScienceDirect.
Dacryocystectomy with Lacrimal Silicone Intubation in Challenging Patients Affected by Recurrent Dacryocystitis and Epiphora: Expanding Minimally Invasive Approach Indications
Abstract
Objective:
In this study, we evaluated the feasibility and safety of dacryocystectomy associated with lacrimal intubation, for the treatment of recurrent dacryocystitis and epiphora secondary to lacrimal obstruction with compromised lacrimal sac, was evaluated.
Subjects and Methods:
32 patients underwent dacryocystectomy with Crawford tubes canalicular insertion, performed by a single surgeon. Post-operative visits were scheduled at 1st and 10th day, 1, 3, and 6 months. At each follow-up visit, the prevalence of epiphora and dacryocystitis was evaluated and compared with baseline data. Also, we evaluated the prevalence of local and systemic post-operative adverse events during the follow-up period.
Results:
11 patients (34.38%) reported persistent epiphora, which lasted for 30 days after surgery. Among them, 9 subjects (28.13%) complained occasional epiphora even at the six months follow-up. In the event of dacryocystitis or subacute phlogosis before surgery, patients reported a definitive symptom resolution. Other reported adverse events were epithelial corneal erosion due to Crawford tube protrusion (4 cases, 12.5%), a Crawford tube extrusion case (3.13%), 3 cases of surgical wound dehiscence (9.36%), and a case of mild local bleeding persisting for 15 days
Conclusion:
A significative epiphora reduction was observed after surgery with an acceptable safety profile, expanding dacryocystectomy indications. This procedure provides a satisfactory resolution of recurrent dacryocystitis. However, this approach should be performed only in well-selected cases: elderly/frail patients with altered lacrimal sacs, epiphora associated with recurrent infections, and failure after dacryocystectomy.
1. INTRODUCTION
Epiphora (excess of lacrimation) is often caused by an acquired nasolacrimal duct obstruction, especially in elderly people, with possible mucopurulent discharge. In fact, recurrent, subacute, or chronic dacryocystitis may occur as a consequence of nasolacrimal duct (NLD) obstructions. Patients may complain about various symptoms, such as epiphora, angular conjunctivitis, canaliculitis, dacryocystitis, or cutaneous fistula.
Most patients who do not exhibit symptomatic improvements with conservative treatment (warm wet packs, lacrimal duct massage/irrigation, broad spectrum antibiotics, local or systemic anti-inflammatory drugs) are addressed to surgical treatment. The first line surgery for these conditions is represented by dacryocystorhinostomy (DCR), performed with transcutaneous (external DCR) or endonasal technique. This technique is usually associated with lacrimal intubation and has variable success rates.
Functional lacrimal duct intubation is usually related to better outcomes after external DCR, although there may be discordant views on the retention of these conformers [1, 2]. Stent insertion is needed in patients with lacrimal stenosis because DCR alone does not restore a sustained reopening. Moreover, it facilitates post-operative healing and prevents fibrotic closure. Longari et al. reported that the decision to apply stent intubation should be performed on the basis of pre-operative findings [3]. Baek et al. reported that complete success after endoscopic DCR, followed by silicone stent intubation, is achieved in 29 out of 31 eyes (93.5%) [4]. However, epiphora and repeated inflammation can occur again after stent removal.
Prior to DCR development in 1904, recurrent or chronic dacryocystitis was treated with dacryocystectomy (DCT). DCT was described, for the first time, by Thomas Woolhouse in 1724 and represented the standard therapy for the management of dacryocystitis and lacrimal fistulas before the advent of DCR [5]. With the spreading of dacryocystorhinostomy, DCT has been considered a minor procedure and, therefore, it is rarely mentioned in recent literature and not adequately considered in the current surgical armamentarium.
Nowadays, the main application of dacryocystectomy is mostly limited to cases of lacrimal sac tumors [6]. Other indications include recurrent dacryocystitis, frail patients with severe systemic affections, nasal or facial malformations, risk of post-DCR nasocutaneous fistula, Wegener granulomatosis (or other forms of vasculitis), and patients that are anxious or unfitting for long-time surgical procedures in a supine position. However, various studies show that in case of NLD obstruction associated with dry eye, ocular scarring pemphigoid, Crohn's disease, and systemic lupus, DCT can be considered a viable alternative [7]. These indications suggest the requalification and reallocation of this procedure among the current surgical options of the lacrimal drainage system.
In this study, dacryocystectomy, featuring permanent lacrimal intubation, is proposed for the treatment of recurrent dacryocystitis secondary to lacrimal obstruction with compromised lacrimal sac, in order to evaluate feasibility, safety, and the possibility of positive outcomes in terms of epiphora and infection resolution.
2. METHODS
32 patients affected by epiphora associated with lacrimal obstruction and chronic or recurrent dacryocystitis were recruited in this single-arm interventional study. Population characteristics are summarized in Table 1. Several patients were recruited because they were over 80 years old, in anticoagulant therapy and did not intend to undergo DCR under general or local anesthesia. Each patient received pre-operative clinical evaluation, including slit lamp examination, visual acuity evaluation, applanation tonometry, lacrimal irrigation, and photographic documentation at the slit lamp. (Table 2)
Then, each patient underwent dacryocystectomy with lacrimal intubation, performed by the same operator in all cases as reported below:
- Skin disinfection with povidone-iodine;
- Anesthesia with subcutaneous and peribulbar infiltration of Lidocaine 2%;
- Cutaneous incision of 10-12 mm at 3-4 mm from the inner cantus along the anterior lacrimal crest;
- Intraoperative assessment of anatomical relationships and conditions of the lacrimal sac;
- Intraoperative assessment of bone conditions (focusing on its alignment and distance with the lacrimal sac);
- Removal of the lacrimal sac (carried out after a H-shaped incision, preferred when possible according to sac conditions found through surgical exploration);
- Anti-inflammatory and antibiotic prophylaxis through lacrimal pathways and intraorbital space irrigation with cefuroxime (50 mg/0.5 ml) and betamethasone (4 mg/2 ml);
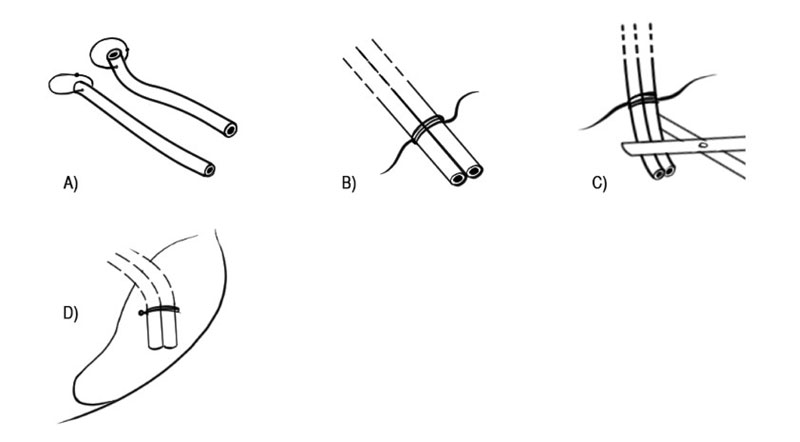
- Intubation of the upper and lower lacrimal canaliculi with a Crawford tube shortened to a length of approximately 10 mm from the distal end of the lacrimal canaliculi. The distal adjusted length of the Crawford tube could be different in accordance with the anatomical surgical findings, avoiding excessive lengths to reduce the risk of tube extrusion;
- Knotting of the two Crawford tube distal heads with a prolene 6-0 thread, followed by shortening of the tube (if not performed before);
- Suture of the tied distal tube heads with anchorage to the posterior intraorbital portion (Fig. 1);
- Placement of free intraorbital Crawford tube ends after realization of a proper deep posterior intraorbital space through careful posterior mucosa disconnection, diathermy, and cauterization directed towards the ethmoidal region.
- Intradermal suture of the nasal cutaneous surgical wound with nylon 6-0 or prolene 6-0 thread;
- Crawford tube excision with scissors at the level of lacrimal puncta, followed by suture of the proximal end on lacrimal puncta with Sharpoint ™ nylon microsuture (nylon 10-0).
| PATIENTS | Men | 10 (26.09%) |
|---|---|---|
| - | Female | 29 (73.91%) |
| - | Total | 39 |
| AGE | Average | 75,52 |
| - | Range | 52-85 |
| - | Patients >80 years old Patients >75 years old |
12 (30.43%) 9 (21.74%) |
| PRINCIPAL DISEASE | Recurrent dacryiocistits | 39 (100%) |
| - | Lachrymal stenosis | 22 (56.41%) |
| - | Epiphora | 39 (100%) |
| ASSOCIATED DISEASES | Blood hypertension | 24 (60.87%) |
| - | Hyschemic cardiopathy Pacemaker holder |
9 (21.74%) 3 (8.70%) |
| - | In therapy with oral antiaggregant | 10 (26.09%) |
| - | In therapy with oral anticoagulants | 5 (13.04%) |
| - | Hypothyroidism | 2 (4.35%) |
| - | Benign Prostatic hypertrophia | 5 (13.04%) |
| - | Diabetes | 15 (39.13%) |
| DCR | DCT with intubation | - |
|---|---|---|
| - ELDERLY PATIENTS (>75) | - ELDERLY PATIENTS (>75) | - |
| HIGH RISK OF HAEMMORRAGE | - LOW PAIN THRESHOLD | - |
| - NO DACRYOCISTITIS EPISODES | - HIGH RISK OF HAEMMORRAGE | - |
| - SINGULAR NASOLACRIMAL DUCT OBSTRUCTION | - MIDFACE BONES ALTERATIONS | - |
| - | - RECURRENT DACRYOCISTITIS | - |
| - | - | > 2 episodes in 6 months |
| - | - | > 3 episodes in 12 months |
| - | -PREVIOUS DCR FAILURE | - |
All intraoperative clinical assessments were performed through a surgical microscope with a focal length of 300 mm. Following surgery, each patient received netilmicin+dexamethasone eye drops, 4 times daily in the treated eye, and heparin sodium 500,000 UI/100 ml eye drops (to prevent hematic clot formation inside the stent), twice a day, for a total of 15 days. Subsequent washings with physiological or medicated solutions are not necessary since the lacrimal pathways remain open and antibiotic eye drops irrigate the tubes anchored to the two lacrimal puncta reaching the nasal orbit. Each patient also applied an Ofloxacin 0.3% ointment 3 times a day on the skin wound for 15 days.
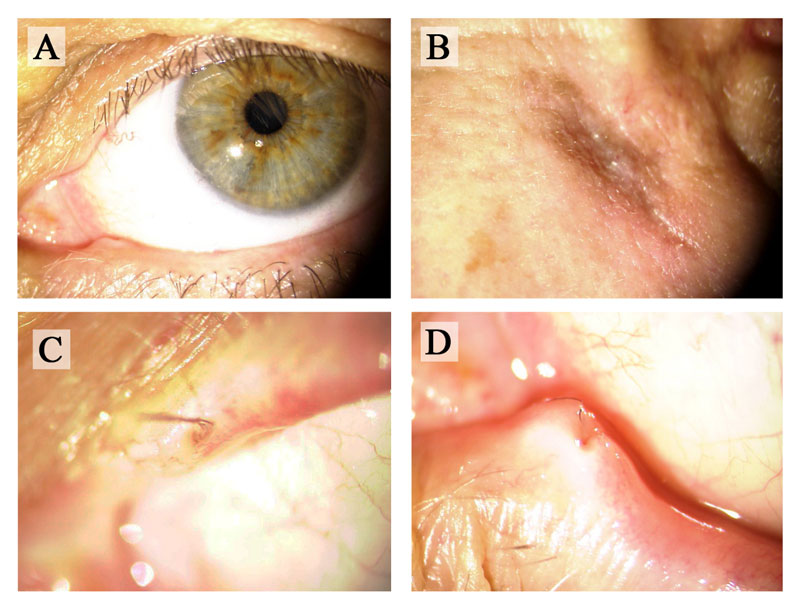
Each patient was subjected to post-operative follow-up after 1 day, 10 days, 1 month, 3 months, and 6 months after surgery. During these visits, complete ophthalmological evaluations were carried out and photographs of clinical presentation were acquired at the slit lamp (Fig. 2). Sutures applied to the skin wound and at the level of lacrimal puncta were removed at 10 days after surgery. No signs of scarring were observed at the level of the lacrimal puncta after removal of Sharpoint ™ Nylon suture. At each follow-up visit, the onset of dacryocystitis recurrence, local or systemic adverse events and the prevalence of epiphora in comparison with the pre-operative time were registered. Statistical significance of differences between the pre- and post-operative time was estimated with the Fisher Exact Test. Irrigation, as well as probing of the lacrimal system, was never performed since it was considered contraindicated for the presence of the stent.
3. RESULTS
11 patients (34.38%) reported the persistence of the epiphora, which lasted for not more than 30 days after surgery. Out of these patients, 9 (28.13%) complained occasional epiphora even at the six months follow-up, albeit markedly reduced if compared to the immediate post-operative time and not assessed during the ophthalmological evaluation. The reduction of epiphora after surgery was statistically significant (p<0.05). In the event of dacryocystitis before surgery, no recurrence was observed throughout post-operative follow-up and all patients reported complete symptoms resolution.
Recorded adverse events consisted of:
- Epithelial corneal erosion for protrusion from the canaliculi of a single Crawford tube (4 cases, 12.5%);
- A complete, post-traumatic, Crawford tube extrusion case (3.13% of operated patients);
- 3 cases of surgical wound dehiscence (9.36%);
- A mild local bleeding case, persisting for 15 days.
Crawford tube protrusion cases were managed by remodeling the tube during the first follow-up visit to eliminate contact with the corneal surface, and in no case, additional surgical treatment or surgical conversion was necessary. The only case of persistent bleeding occurred in a patient taking acetylsalicylic acid 100 mg/day and no hospitalization or other forms of tamponing were required as it was minimal bleeding. No adverse events, general or local, were recorded during the follow-up.
4. DISCUSSION
DCR success rates are very high (95% -97%) for the treatment of epiphora and mucopurulent secretion [8]. However, success rates for endoscopic DCR are reported to vary between 65% and 97% [9, 10]. In a recent review of Tooley et al. collecting real-life data, an 86% DCR success rate was reported in young patients, while it was drastically reduced to 64% in patients over 80 years of age [11]. In these subjects, it is definitely more desirable to perform the DCR endoscopically, given the lower invasiveness of the intervention compared to the external DCR, but in an elderly patient or in a patient with a higher risk of bleeding, especially in case of cardiopathic patients taking anticoagulant therapy, any eventual bleeding at the nasal cavity level can lead to blurring of the endoscopic visualization, with prolongation of surgical maneuvers or even abrupt interruption of the operation.
Moreover, the rate of severe complications is higher in the elderly population. Tooley et al. reported a higher rate of severe adverse events in older people (including stroke, myocardial infarction, syncope, and severe hemorrhage) in comparison with the younger cohort (15% vs. 2%) [11]. Elderly patients were also less likely to experience symptomatic relief.
Multiple factors increase surgical risk in elderly patients, including functional decline, reduced reserve capacity, polytherapy, and concomitant comorbidity. Various studies have shown that older age is an independent risk factor for perioperative complications and post-operative mortality [12-14]. Increased surgical risk in the elderly is present for both complex operations and less complex procedures, such as cataract surgery [15].
In all cases of high risk DCR, functional lacrimal intubation is advisable. Moreover, in the case of canalicular obstruction, permanent lacrimal intubation may be needed to prevent stenosis recurrence that could occur post-removal. It is typical in the DCR to insert a single tube that crosses the 2 lacrimal puncta to form a horseshoe loop that connects the two upper and lower tear drainage systems; the positioning of this device requires the execution of numerous physiological solution washes to keep the conduit, clean and sterile, because the lack of opening at the level of the lacrimal puncta does not allow the direct flow of antibiotic eye drops into the tube; moreover, it could cause conjunctival, corneal and cutaneous lesions of the internal canthus and nasal bones.
The lacrimal sac may be found reworked, inconsistent, atresic or infected, with poor and deteriorated mucosa consistency, especially in patients with recurrent dacryocystitis (more than two episodes in 6 months or three episodes in one year), with granulomatous diseases affecting the nasolacrimal pathways and/or with malformations of the midface bones (the nasal, ethmoid, zygomatic and maxillary ones). These factors may affect the success of DCR procedures, and patients who do not achieve resolution of recurrent dacryocystitis, even after a technically correct DCR, may benefit from a complete lacrimal sac removal. In most cases, infections of the lacrimal system originate at the obstructed distal end with bacterial overlapping at the level of the lacrimal sac and following sac alterations (such as progressive sac dilation). Therefore, complete removal can avoid future recurrence of inflammation and infections involving the lacrimal sac. Moreover, since a nasal anastomosis is not needed in DCT, another possible “iatrogenic” origin site for infections (facilitated by the communication with nasal mucosa) [16] is eliminated, which is instead created by the osteotomy necessary to perform DCR.
In case of unsuccessful DCR, a conjunctivo dacryocystorhinostomy with Jones tube placement can also be performed as an additional surgery. This technique is associated with reported success rates between 75% and 78.6% after 6 months [17, 18]. In this paper, a modified dacryocystectomy associated with lacrimal intubation with Crawford tubes, which can be considered as an alternative procedure with respect to conjunctivo dacryocystorhinostomy, is described. In this study, with a 71.87% success rate after six months, slightly lower results were obtained, if compared with conjunctivo dacryocystorhinostomy success rates. However, even in case of functionally successful conjunctivo dacryocystorhinostomy, post-operative dissatisfaction can be significant, especially in patients with 70 years of age or older, making this option recommended only in cases of exceptionally remarkable symptoms for these age groups [19]. Patient dissatisfaction after successful conjunctivo dacryocystorhinostomy, is often related to non-tolerated complications, such as conjunctival granuloma, canthal deformity, Jones’s tube migration or clogging (with the frequent need of repeated irrigations), infection or chronic pain. In contrast, post-operative complications observed after DCT with lacrimal intubations were rare and not severe, making this min-invasive alternative generally well-tolerated, even in elderly patients. Moreover, post-operative lacrimal irrigation was not necessary and no infective events were observed.
In this study, complete resolution of dacryocystitis and mucopurulent discharge was obtained after DCT in all patients. Moreover, lacrimal functional intubation, which is not ordinarily provided for in this surgical technique, was applied to create permanent drainage in the intraorbital region, in order to improve dacryocystectomy outcomes in reducing epiphora. However, the lacrimal sac removal interrupts drainage into nasal cavities. This “lacrimal plug” effect is particularly desirable in patients with different degrees of dry eye because it increases lacrimal meniscus, improving keratoconjunctivitis sicca or tear hyposecretion [20]. In fact, Boynton and Anawis commented that in the elderly with dry eye, DCR can fail, even when technically correct, because these individuals have insufficient lacrimal production to maintain the lacrimal flow [21].
Among all patients, although some of the subjects undergoing DCT with intubation showed a slightly increased lacrimal meniscus, epiphora was not clinically detectable. This phenomenon can be explained by improved drainage provided by the permanent silicone intubation and the realization of an alternate tear outflow route in the posterior orbit, with a diffusion mechanism. For these reasons, the silicone tube should not be removed in the absence of patient complaints or adverse events. Moreover, permanent intubation maintains the canalicular patency, counteracting a possible following stenosis due to inflammatory reactions. In one of the cases of persistent epiphora detected in this study, the patient presented a malposition of the lower lacrimal punctum, influencing the normal tears outflow. The subject was then addressed to a surgical resolution of the preexisting lid condition by lateral tarsal strip.
Complications following dacryocystectomy are rare. Accidental angular vein injury may lead to important bleeding. Other complications include dehiscence of the surgical wound, wound infection, increased lacrimal meniscus and epiphora, recurrent dacryocystitis (in case of incomplete removal of lacrimal sac), and a facial scarring/cheloid [20]. Although very rare, 2 cases of visual loss and 1 case of orbital cellulitis, following a DCT, have been reported in the literature [20, 22]. A possible cause could be the violation of the periorbita and orbital septum during surgery, resulting in orbital bleeding and hematoma with optic nerve compression and visual loss. Pyogenic granuloma cases did not occur among the participants in this study. Even with the presence of permanent communication between the ocular surface and the deep orbital region, events of orbital cellulitis or other signs of infections have not been observed in the post-operative time. Moreover, prophylaxis of post-operative infections was performed in the course of surgery through repeated antibiotic and anti-inflammatory irrigation associated with accurate cauterization in the posterior orbital space.
Crawford tube prolapse is one of the most common complications when silicone intubation is applied. A review of literature by Brookes and Olver reports the incidence of tube prolapse after DCR between 1.5% and 14% [23]. Risk factors for tube prolapse include lower eyelid laxity, low suture apposition, and types of thread used. The lateral prolapse of the tube is problematic, given the potential corneal and conjunctival erosion, punctal erosion, and patient discomfort [24]. The concern for the development of these complications, which is shared by both patient and surgeon, often leads to premature removal of the tube.
In this study, Crawford tubes were chosen since their metal end can be exploited to facilitate their introduction in lacrimal canaliculi. Crawford tubes’ intraorbital anchorage is a safe procedure as it limits the anterior dislocation with no risk of ocular extrinsic muscle involvement. The 10-0 nylon (with Sharpoint ™ needle) suture on the lacrimal puncta has the advantage of maintaining canalicular positioning (supporting the intraorbital suture). Adverse reactions at the punctal level had been controlled with the application of topical medications in the following post-operative follow-up. In addition, no scarring or laceration to the puncta were observed. Suture of the tubes at the level of the superior and inferior lacrimal puncta was performed to avoid dislocation, conjunctival and corneal epithelial insults, which are common when continuous silicone intubation is applied. After canalicular suture removal, no cases of inner tube displacement were observed, probably due to stable tube intraorbital anchorage and the implanted tube length, preventing lower dislocation with gravity. However, extrusion of the silicon tubes occurred in some of the patients under examination.
During follow-up, no cases of canalicular inflammation and granuloma formation were registered. Moreover, with the passage of the nylon thread inside the drainage tube lumen, it is possible to avoid occlusion by debris, mucous swelling, or clots due to post-operative bleeding. Silicone tube obstruction is also prevented by the application of heparin eyedrops in the treated eye, reducing intraluminal blood coagulation.
In dacryocystectomy associated with permanent intubation, in case of intraorbital adverse reactions, secondary infections or patients’ complaints (despite the repeated application of intraoperative steroid and antibiotic drugs), removal of lacrimal intubation is still possible at a later time, after removal of punctal suture. In cases of properly placed intubation, no infections or inflammatory orbital disorders have been observed till now.
Given these considerations, the choice between DCR or DCT may also be influenced by different lacrimal system conditions assessed intraoperatively: proximal lacrimal stenosis (at the level of the canaliculi or their conjunction with the lacrimal sac), repeated infectious events of the lacrimal sac or mucopurulent discharge at the time of intraoperative irrigation of lacrimal system, can lead the surgeon choice towards a dacryocystectomy with intubation procedure.
DCT combined with tubes insertion can be taken into consideration in other selected cases, such as in frail patients with severe dry eye and chronic dacryocystitis, patients with low pain threshold, patients with hemorrhagic diathesis or coagulopathy, scarring or granulomatous diseases (ocular pemphigoid, Wegener's granulomatosis, systemic lupus, etc.), cardiovascular or neurological comorbidities, severe infections, nasal malformations, mucoceles, tumors or malformations of the lacrimal sac [20, 25, 26].
However, if the lacrimal sac is not involved by infections or chronic inflammation, and is found in acceptable conditions in the intraoperative setting, a dacryocystorhinostomy should always be preferred.
CONCLUSION
DCT associated with lacrimal intubation should be considered only in selected cases. In this study, DCT appears to be a valid surgical alternative to the more invasive DCR in low pain threshold patients, in elderly subjects (75 years and older) with a high risk of bleeding and/or on anticoagulant therapy, but especially in patients with recurrent dacryocystitis (more than 2 in 6 months and/or more than 3 in one year), which drastically reduce safety and chances of success, as well as increase the risk of DCR complications. DCT indications can be expanded, including epiphora, when functional lacrimal intubation is applied. Current dacryocystectomy indications are limited to the treatment of lacrimal sac tumors, however, the application of permanent silicon intubation (which can be removed in case of discomfort or lack of patients’ compliance) may improve the outcomes regarding the resolution of epiphora. In fact, functional intubation can improve DCR and DCT outcomes, particularly in patients above 80 years of age with proximal stenosis and/or lacrimal sac alteration [10, 11, 27, 28].
DCT differs from DCR since it is less invasive, does not include an osteotomy or lesions to the nasal mucosa, with a lower risk of severe hemorrhage or ascending infections with intranasal origin. This modified DCT procedure provides a satisfactory resolution of recurrent dacryocystitis, which may be superior if compared to lachrymal endoscopy (since it usually does not include the asportation of the lachrymal sac) [29, 30].
Dacryocystorhinostomy still remains the first choice of surgery for distal nasolacrimal duct obstruction and if the lacrimal sac is unaffected; however, DCT with intubation, when well indicated (especially after the assessment of clinical findings in the intraoperative setting), can be decisive in the resolution of chronic dacryocystitis, avoiding severe intra- and post-operative complications, in selected patients.
LIST OF ABBREVIATIONS
| DCR | = Dacryocystorhinostomy |
| DCT | = Dacryocystectomy |
| NLD | = Nasolacrimal Duct |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study was reviewed and approved by the Institutional Review Board of Institute of Ophthalmology, Turin, Italy.
HUMAN AND ANIMAL RIGHTS
All procedures performed in this study involving human participants were in accordance with the institutional ethical board standards and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained in written form from all individual participants included in the study.
CONSENT FOR PUBLICATION
Informed consent was obtained in written form from all individual participants included in the study.
AVAILABILITY OF DATA AND MATERIALS
The data generated and analyzed during this study are stored in the repository of the Department of Surgical Sciences of the University of Turin, and can be provided upon reasonable request addressed to the corresponding author [R.N].
FUNDING
None.
CONFLICT OF INTEREST
The author declares no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
All materials needed in this study have been procured by the Eye Clinic Section, Department of Surgical Sciences, University of Turin.


