All published articles of this journal are available on ScienceDirect.
Ocular Manifestations in Patients with Coronavirus Disease 2019 (COVID-19): A Real World Multicenter Observational Study in Egypt
Abstract
Background:
The aim of the work was to evaluate the ocular manifestations in the patients with COVID-19 and its role in the prediction of the course and the outcome of the disease.
Methods:
This retrospective study was conducted at two tertiary referral COVID-19 isolation hospitals in two major university hospitals in Egypt. Two hundred and twenty-eight patients were enrolled in the study. The medical records of patients who had clinically confirmed COVID-19 between 1/5/2020 to 15/7/2020 were retrospectively reviewed. Data were collected from patient charts, including age, sex, accommodation, ocular manifestations, fever, headache, cough, dyspnea, anosmia, cyanosis, abdominal pain, anorexia, liver, kidney, cardiac manifestations, CT, X-ray finding, blood tests, and outcome of the disease.
Results:
Thirty-four patients with ocular manifestation were finally enrolled in the study with a mean age of 42.1 years; 20 patients (58.8%) were men. The incidence of ocular manifestation was 14.9% (34/228). All patients with ocular manifestations had conjunctivitis (redness, epiphora, foreign body sensation), which had been treated and resolved completely within 10 days in all patients without any permanent ocular damage. There was a trend between the presence of ocular manifestations and the associated milder disease course, although this trend was not statistically significant.
Conclusion:
Ophthalmic manifestation is common in patients with COVID-19 and it occurs more frequently in patients with mild to moderate form of COVID-19, but it could not predict the patient’s mortality.
1. INTRODUCTION
Coronavirus disease 2019 (COVID- 19) has been reported to start in Chinese patients. Currently, the disease is spreading rapidly around the world. The pathogen for COVID-19 is a new coronavirus (SARS-CoV-2 Coronavirus), which has been identified as a member of the Coronaviridae family. Another member of this family called SARS-CoV-1 was responsible for severe acute respiratory syndrome. When compared to SARS-CoV-1, SARS-CoV-2 has a similar binding receptor, similar systemic features, and epidemiological specific characteristics [1-11].
Although up till now, it is not evinced that infection with SARS-CoV-1 was associated with conjunctivitis, some reports have confirmed the eye as a possible site of virus transmission [12].
There are few reports in the medical literature that identify the ocular manifestation of SARS-CoV-2 [13]. Moreover, researchers have not reported the significance of these ocular finding in predicting the course of the disease. So, the aim of this study was to evaluate the ophthalmological involvement in patients confirmed to have COVID-19 and its rule in the prediction of the course of the disease.
2. METHODS
This retrospective study was carried out at isolation hospitals in the faculty of medicine, Tanta University and Ain-shams University, Egypt. It was conducted according to the principles of the Helsinki Declaration and was approved by the ethical review board of both faculties. Personal data of the participants were kept confidential and used only for research purposes. Results and images were collected from the patients after their consent. Consent was taken from the patient to post the image included in the manuscript.
The medical records of patients who had been laboratory confirmed to be positive for COVID-19 between 1/5/2020 to 15/7/2020 were reviewed. The collected data included sociodemographic data such as age, sex, and residence. Medical, laboratory, and radiological data were also reviewed for the presence of fever, headache, cough, dyspnea, anosmia, cyanosis, abdominal pain, anorexia, hepatic, renal, or cardiac manifestations. Computerized tomography (CT) and X-ray chest findings were also recorded. Blood tests results, including red blood cells, white blood cells, platelets, hemoglobin concentration, the international normalized ratio (INR), D dimer, and the outcome of the disease were also collected.
Ocular manifestations for any ocular symptoms or any signs suggestive of viral infection like conjunctival hyperemia, epiphora, lid edema, irritation, or foreign body sensation were also recorded.
The severity of COVID-19 disease was clinically evaluated and mild stage was characterized by the absence of pneumonia and hypoxia. Meanwhile, moderate stage was characterized by the presence of pneumonia in the absence of the criteria of the severe stage. The severe form of the disease was characterized by the presence of any of the following: oxygen saturation less than 90%, involvement of more than 50% of lung field, a respiratory rate more than 30 cycles per minute, or any of the manifestations of respiratory distress.
2.1. Statistical Analysis
The collected data were tested for normality by Shapiro Wilks test. Normally distributed quantitative data were expressed in the form of mean and Standard Deviation (SD), while skewed quantitative data were expressed in the form of median and range. Categorical data were expressed in the form of number (No.) and percentage (%). Student’s t-test was used for comparison of normally distributed quantitative variables, while Mann Whitney's test was used for comparison of abnormally distributed ones. Chi-square test (χ2) was used for comparison of categorical variables and whenever any of the expected cells were less than five, Fischer’s Exact test was used. Logistic regression was used to ascertain the effect of the possible risk factors on the mortality of the included patients. Two-sided P- value of < 0.05 was considered statistically significant. All the analyses were performed using SPSS statistical package version 23 (SPSS Inc. Released 2015. IBM SPSS statistics for windows, version 23.0, Armnok, NY: IBM Corp).
3. RESULTS
Two hundred and twenty eight charts (228) of COVID-19 patients were included in this study. Among them, 34 patients (14.9%, 95% CI: 10.1-19.7%) showed ocular manifestations. The ocular manifestation that was present in all the affected patients was conjunctivitis manifested by conjunctival hyperemia, epiphora, lid edema, and foreign body sensation (Fig. 1).
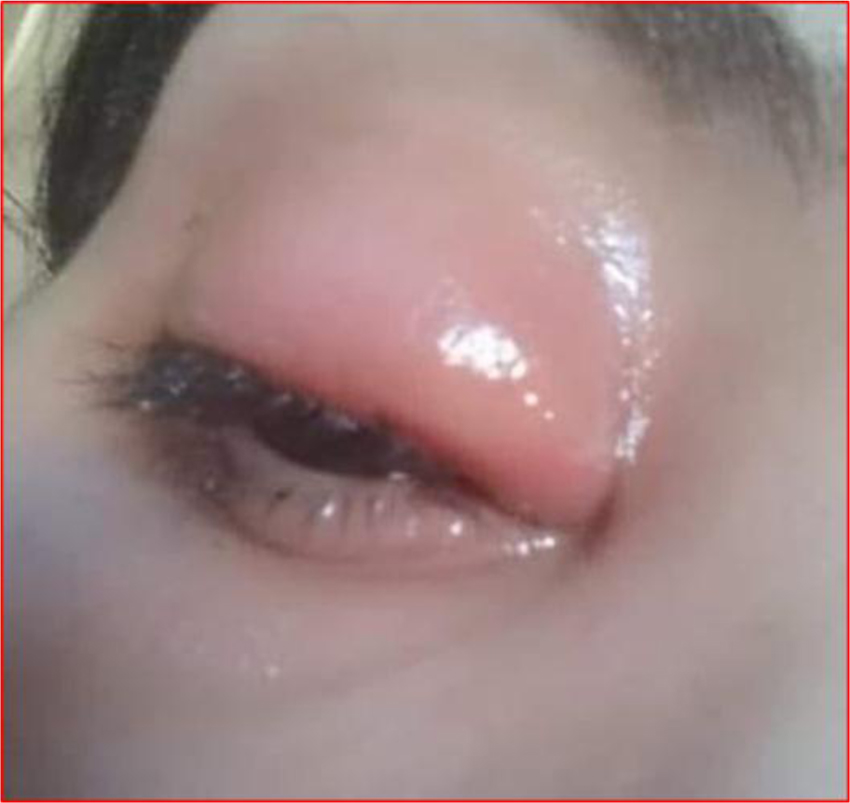
There was no significant difference between the group of patients with ocular manifestations and the group without ocular manifestation regarding age, gender, residence, body mass index, or comorbidities. However, smoking was significantly more prevalent among patients with ocular manifestations (P= 0.006) (Table 1).
None of COVID-19 related symptoms or signs were significantly associated with the presence of ocular manifestation. The clinical course of the disease was not significantly associated with the presence of ocular manifestations either. Noone with ocular manifestations in this study died, however, there was no significant difference between patients with or without ocular manifestations as regards the mortality rate (P=0.137) (Table 2). Patients with and those without ocular manifestation were comparable as regards the laboratory findings (Table 3).
| Character | Ocular Manifestations | Total (n=228) | P Value | |
|---|---|---|---|---|
|
Yes (n=34) |
No (n=194) |
|||
| Age (y) Mean ±SD |
42.06 ± 16.41 | 42.18 ± 13.27 | 42.16 ± 13.91 | 0.122 |
| Gender Male Female |
20 (58.8%) 14 (41.2%) |
107 (55.2%) 87 (44.8%) |
127 (55.7%) 101 (44.3%) |
0.713 |
| Residence Rural Urban |
20 (58.8%) 14 (41.2%) |
139 (71.6%) 55 (28.4) |
159 (69.7%) 69 (30.3%) |
0.133 |
| Smoking | 19 (55.9%) | 61 (31.4%) | 80 (35.1%) | 0.006 |
| Comorbidity No Hepatic Renal HTN & Cardiac Diabetes |
18 (52.9%) 2 (5.9%) 2 (5.9%) 6 (17.6%) 6 (17.6%) |
149 (76.8%) 8 (4.1%) 4 (2.1%) 17 (8.8%) 16 (8.2%) |
167 (73.2%) 10 (4.4%) 6 (2.6%) 23 (10.1%) 22 (9.6%) |
0.062 |
| BMI Normal Overweight Obese Morbid obesity |
2 (5.9%) 12 (35.3%) 17 (50%) 3 (8.8%) |
10 (5.2%) 106 (54.6%) 69 (35.6%) 9 (4.6%) |
12 (5.3%) 118 (51.8%) 86 (37.7%) 12 (5.3%) |
0.120 |
| Manifestations | Ocular Manifestations | Total (n=228) | P Value | |
|---|---|---|---|---|
|
Yes (n=34) |
No (n=194) |
|||
| Fever No Mild High |
14 (41.2%) 12 (35.3%) 8 (23.5%) |
88 (45.4%) 68 (35.1%) 38 (19.6%) |
102 (44.7%) 80 (35.1%) 46 (20.2%) |
0.845 |
| Headache | 12 (35.3%) | 72 (37.1%) | 84 (36.8%) | 0.839 |
| Sore throat | 7 (20.6%) | 44 (22.7%) | 51 (22.4%) | 0.787 |
| Cough No Mild Continuous |
27 (79.4%) 5 (14.7%) 2 (5.9%) |
150 (77.3%) 32 (16.5%) 12 (6.2%) |
177 (77.6%) 37 (16.2%) 14 (6.1%) |
0.962 |
| Dyspnea No Mild Continuous |
12 (35.3%) 15 (44. %1) 7 (20.6%) |
70 (36.1%) 86 (44.3%) 38 (19.6%) |
82 (36%) 101 (44.3%) 45 (19.7%) |
0.990 |
| Anorexia | 11 (32. %4) | 69 (35.6%) | 80 (35.1%) | 0.717 |
| Anosmia | 11 (32.4%) | 67 (34.5%) | 78 (34.2%) | 0.805 |
| Pallor | 1 (2.9%) | 9 (4.6%) | 10 (4.4%) | 0.656 |
| Fatigue | 19 (55.9%) | 108 (55.7%) | 127 (55.7%) | 0.982 |
| Vomiting | 7 (20.6%) | 42 (21.6%) | 49 (21.5%) | 0.889 |
| Diarrhea No 3-6 times >6 times |
18 (52.9%) 15 (44.1%) 1 (2.9%) |
108 (55.7%) 80 (41.2%) 6 (3.1%) |
126 (55.3%) 95 (41.7%) 7 (3.1%) |
0.952 |
| Abdominal pain | 6 (17.6%) | 36 (18.6%) | 42 (18.4%) | 0.90 |
| Clinical course Mild Moderate Severe |
27 (79.4%) 5 (14.7%) 2 (5.9%) |
114 (58.8%) 53 (27.3%) 27 (13.9%) |
141 (61.8%) 58 (25.4%) 29 (12.7%) |
0.080 |
| O2 saturation 100-95% 95-90% <90% |
24 (70.6%) 8 (23.5%) 2 (5.9%) |
134 (69.1%) 44 (22.7%) 16 (8.2%) |
158 (69.3%) 52 (22.8%) 18 (7.9%) |
1.00 |
| Outcome Survived Died |
34 (100%) 0 (0%) |
180 (92.8%) 14 (7.2%) |
214 (93.9%) 14 (6.1%) |
0.137 |
| Lab. Findings | Ocular Manifestations | Total (n=228) | P Value | |
|---|---|---|---|---|
|
Yes (n=34) Mean ±SD |
No (n=194) Mean ±SD |
|||
| Hb | 13.12 ± 2.12 | 13.08 ± 2.07 | 13.09 ± 2.07 | 0.923 |
| Platelets | 232.67 ± 84.29 | 225.78 ± 82.93 | 226.80 ± 82.98 | 0.625 |
| WBCs | 5.80 ± 3.88 | 5.52 ± 3.20 | 5.56 ± 3.30 | 0.989 |
| Lymphocytes | 36.58 ± 21.91 | 35.10 ± 20.78 | 35.32 ± 20.90 | 0.758 |
| Direct bilirubin | 0.27 ± 0.17 | 0.29 ± 0.18 | 0.28 ± 0.18 | 0.447 |
| Indirect bilirubin | 0.52 ± 0.17 | 0.51 ± 0.17 | 0.51 ± 0.17 | 0.767 |
| Albumin | 4.07 ± 0.46 | 4.02 ± 0.50 | 4.03 ± 0.49 | 0.628 |
| ALT | 29.71 ± 16.28 | 30.02 ± 16.09 | 29.97 ± 16.08 | 0.917 |
| AST | 27.71 ± 9.92 | 28.43 ± 9.74 | 29.97 ± 16.08 | 0.681 |
| INR | 1.06 ± 0.13 | 1.07 ± 0.13 | 1.07 ± 0.13 | 0.745 |
| D dimer | 0.49 ± 0.46 | 0.50 ± 0.47 | 0.50 ± 0.47 | 0.975 |
| LDH | 210.97 ± 144.32 | 207.55 ± 143.71 | 208.06 ± 143.49 | 0.868 |
| Ferritin | 324.20 ± 564.87 | 331.80 ± 570.56 | 330.67 ± 568.48 | 0.076 |
| Creatinine | 0.95 ± 0.24 | 0.94 ± 0.23 | 0.95 ± 0.23 | 0.097 |
| CRP | 14.82 ± 25.54 | 12.22 ± 16.92 | 12.60 ± 18.42 | 0.757 |
Patients with conjunctivitis were treated with topical antibiotics to prevent secondary bacterial infection, topical steroid, and tear substitutes. The viral conjunctivitis in all the affected patients resolved within 10 days with complete recovery of ocular symptoms and signs without any permanent ocular damage. The presence of ocular manifestations was not a significant predictor of the patients’ mortality. The percentage of oxygen saturation was the only significant predictor for the patients’ mortality (Table 4).
4. DISCUSSION
A very few articles have assessed the ophthalmological manifestation in patients with SARS-CoV-1 or SARS-CoV-2 infection. To our knowledge, none of these reports have evaluated the prognostic value of these findings. Our article aimed to evaluate the ocular finding of COVID-19 during the pandemic period in two big isolation hospitals in Egypt and if these ocular manifestations could help the physician to predict the course of the disease.
| Variables | B | P-Value | OR | 95% CI | |
|---|---|---|---|---|---|
| Lower | Upper | ||||
| Age | 0.012 | 0.542 | 1.012 | 0.974 | 1.052 |
| Gender | -1.13 | 0.089 | 0.323 | 0.088 | 1.190 |
| Smoking | 0.967 | 0.084 | 2.630 | 0.879 | 7.867 |
| ALT | 0.00 | 0.980 | 1.00 | 0.967 | 1.035 |
| Albumin | 0.776 | 0.176 | 2.173 | 0.706 | 6.685 |
| Creatinine | -0.997 | 0.432 | 0.369 | 0.031 | 4.435 |
| Ferritin | -0.001 | 0.565 | 0.999 | 0.998 | 1.001 |
| CRP | -0.015 | 0.554 | 0.985 | 0.939 | 1.034 |
| O2 sat. | 3.490 | <0.001 | 32.79 | 8.634 | 124.548 |
| Comorbidity | -0.505 | 0.157 | 0.603 | 0.300 | 1.215 |
| Ocular manifestation | 18.64 | 0.998 | --- | --- | ---- |
Our results showed that the incidence of ocular manifestation was 14.9% and all the ocular manifestation was in the form of conjunctivitis, which had been treated and resolved completely within 10 days in all patients without any permanent ocular damage. Conjunctivitis is presumed to be self-limited and can be managed with symptomatic care as weak steroid eye drops and lubricant. Antibiotics eye drops were used to prevent secondary bacterial infection. Ocular shedding of SARS-CoV-2 via tears is a distinct possibility of which ophthalmologists should be aware.
According to our findings, the presence of ocular manifestation tends to be associated with mild and moderate cases and with less aggressive course of the disease. Future research is needed to explain the presence of ocular manifestations, mainly in mild and moderate cases.
In a previous report, the incidence of ocular manifestation was found to be 0.8% (9/1099 patients) from 552 hospitals across 30 provinces in China, these ocular manifestations were described as conjunctival congestion [14].
A recent case series from Hubei province, China demonstrated the presence of ocular symptoms in 12 (31.6%) of 38 hospitalized patients with COVID-19. These ocular manifestations included conjunctival hyperemia (3 patients), chemosis (7 patients), epiphora (7 patients), or increased secretions (7 patients) [13]. In addition, Xia et al. [14] reported that out of 30 hospitalized patients with COVID-19, one patient had conjunctivitis.
Retinal changes are also thought to be linked with COVID-19 infection. Subclinical hyper reflective lesions at the level of ganglion cell layer and the inner plexiform layer are found in 12 adults examined using optical coherence tomography after systemic disease onset; cotton wool spots and hemorrhages were found on fundus examinations in 4 of these patients [15]. Invernizzi et al. found retinal hemorrhages (9.25%), cotton wools spots (7.4%), tortuous vessels (12.9%) and dilated veins (27.7%) in 54 patients with COVID-19 upon screening with fundus photography [16]. Lecler et al. showed abnormal MRI findings in the posterior pole of 9 patients with COVID-19 consisting of one or multiple hyper intense nodules in the macular region on FLAIR-weighted images [17]. These lesions were supposed to be either direct inflammatory infiltration of the retina or microangiopathic disease from viral infection.
Limitation of this study: the retrospective nature of the study and lack of posterior segment examination due to the infectious nature of the disease and the increase in the number of patients in the isolation hospital and the increased anxiety of the patients, which prevent the dilatation of pupil and careful examination of the retina and the use of further investigation as optical coherence tomography and fluorescein angiography. Despite above-mentioned limitation, we have described for the first time the ocular manifestation of COVID-19 in the Middle East and Africa, in an effort to inform ophthalmologists and others around the world about the ocular manifestations of COVID-19 and their rule in the prediction of the course of the disease.
CONCLUSION
Ophthalmic manifestation is common in patients with COVID-19 and it occurs more frequently in patients with mild to moderate form of COVID-19, but it could not predict the patient’s mortality.
AUTHORS' CONTRIBUTION
R.G., S.A, M.K, E.E, A.G, and D.E. collected the study data, wrote, revised and approved the manuscript. O.A., H.F., S.S, M.A., M.A., K.O, and D.E. performed the statistical analysis, collected the study data, wrote, revised and approved the manuscript.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The approval was obtained from the ethics committee of Tanta University, Faculty of Medicine, Egypt.
HUMAN AND ANIMAL RIGHTS
No animals were used in this research. All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICTION
An informed consent was obtained from the all participants
STANDARDS OF REPORTING
STROBE guideline has been followed in this study
AVAILABILITY OF DATA AND MATERIALS
Not applicable.
FUNDING
None.
CONFLICT OF INTEREST
Sherief Abd-Elsalam is the Editorial board member of The Open Biomarkers Journal.
ACKNOWLEDGEMENTS
Declared none.


